By:
Published: August, 2023
Medicare is a health insurance program for individuals over the age of 65 and people with disabilities in the United States. It is composed of four parts: Hospital Insurance (HI; Part A), Medical Insurance (Part B), the option for private plans under Medicare Advantage (Part C), and prescription drug coverage (Part D). The program is funded by contributions from employees and employers in the HI Trust Fund (Part A), premiums paid by beneficiaries and general federal revenues in the Supplementary Medical Insurance (SMI) Trust Fund (Parts B and D), or a combination of both (Part C).
The Impact of COVID-19 on the Health of Older Adults
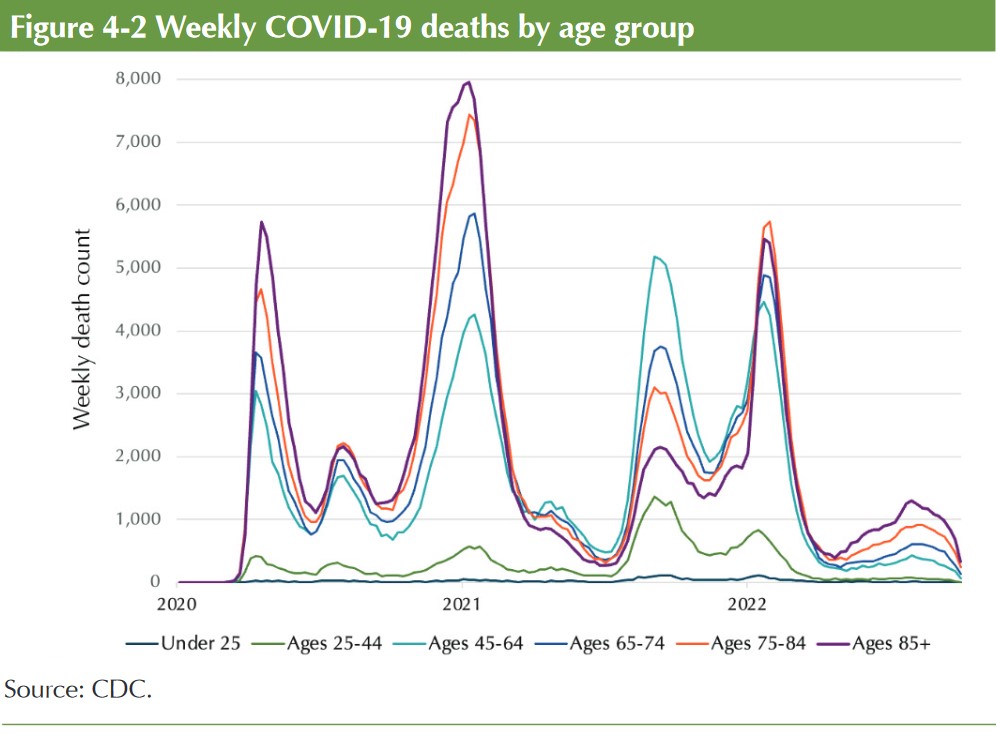
The COVID-19 pandemic had a dramatic impact on older adults in the U.S. Mortality from COVID-19 was highest among individuals aged 75 and older compared to any other age group. By June 2022, approximately one and a quarter percent (1.25%) of adults over age 65 had died due to COVID-19.
Medicare beneficiaries living in nursing homes were 14x more likely to be diagnosed with COVID-19 than beneficiaries living in the community, highlighting in new ways the importance of keeping older adults with care needs in their communities as long as possible.
The Impact of COVID-19 on the Financial Condition of Medicare
Contrary to expectations, the COVID-19 pandemic slightly extended the projected lifespan of the Medicare Hospital Insurance (HI) Trust Fund. Unfortunately, the reasons for this deferral of the trust fund’s depletion date were largely driven by negative health effects on beneficiaries:
- Premature deaths were disproportionately concentrated among Medicare beneficiaries.
- Fears of exposure to, and infection with, COVID-19 while accessing health care facilities and provider offices reduced Medicare spending and claims.
- – As a result, many beneficiaries canceled or deferred health care services.
- – It is unclear what repercussions delayed care will have on beneficiaries’ long-term health.
- Total use of medical care declined despite the increase in access to telehealth services; however, relaxed regulations around the use of telemedicine under Medicare did lead to an increase in the use of telehealth services compared to before the pandemic.
Lessons Learned and Policy Options
- Shore up the solvency of the HI Trust Fund to protect against future economic downturns. [Option 4.B.1]
Policy options include: dedicating new revenues to the HI Trust Fund; reducing spending that fails to increase efficiency or quality of care; and/or infusing general revenue finances into the program. - Better protect provider payments against unexpected errors in inflation projections. [Option 4.B.2]
Currently, Medicare payments to providers increase at a set rate over time. If the projected increase in the costs of care falls short of the real increase in costs, that difference is never made up, leaving providers undercompensated. Payments could be indexed to inflation, like other national fiscal programs (e.g., Social Security), or could incorporate a correction method to adjust for projection errors – which would correct in both directions (e.g., if payments are higher, the rate would be reduced to correct for the error, and vice versa). - Improve access to telehealth services and address the digital divide. [Option 4.F.2]
Congress could consider permanently reducing restrictions around the use of telemedicine, or to at least make those changes automatic in the event of any future public health emergency. Additionally, Congress could consider expanding access to both the tools (phones, computers, internet access) and tech literacy necessary to narrow gaps in access to telehealth services and, hopefully as a result, health disparities.
dddddddddddddddddd